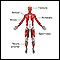
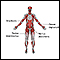
Muscle function loss
Definition
Muscle function loss is when a muscle does not work or move normally. The medical term for complete loss of muscle function is paralysis.
Alternative Names
Paralysis; Paresis; Loss of movement; Motor dysfunction
Considerations
Loss of muscle function may be caused by:
- A disease of the muscle itself (myopathy)
- A disease of the area where the muscle and nerve meet (neuromuscular junction)
- A disease of the nervous system: Nerve damage (neuropathy), spinal cord injury (myelopathy), or brain damage (stroke or other brain injury)
The loss of muscle function after some of these types of events can be severe. In some cases, muscle strength may not completely return, even with treatment.
Paralysis can be temporary or permanent. It can affect a small area (localized or focal) or be widespread (generalized). It may affect one side (unilateral) or both sides (bilateral).
If the paralysis affects the lower half of the body and both legs it is called paraplegia. If it affects both arms and legs, it is called quadriplegia. If the paralysis affects the muscles that cause breathing, it is quickly life threatening.
Causes
Diseases of the muscles that cause muscle-function loss include:
- Alcohol-associated myopathy
- Congenital myopathies (most often due to a genetic disorder)
- Dermatomyositis and polymyositis
- Drug-induced myopathy (statins, steroids)
- Muscular dystrophy
Diseases of the nervous system that cause muscle function loss include:
- Amyotrophic lateral sclerosis (ALS, or Lou Gehrig disease)
- Bell palsy
- Botulism
- Guillain-Barré syndrome
- Myasthenia gravis or Lambert-Eaton Syndrome
- Neuropathy
- Paralytic shellfish poisoning
- Periodic paralysis
- Focal nerve injury
- Polio or other viruses
- Spinal cord or brain injury
- Stroke
Home Care
Sudden loss of muscle function is a medical emergency. Get medical help right away.
After you have received medical treatment, your health care provider may recommend some of the following measures:
- Follow your prescribed therapy.
- If the nerves to your face or head are damaged, you may have difficulty chewing and swallowing or closing your eyes. In these cases, a soft diet may be recommended. You will also need some form of eye protection, such as a patch over the eye while you are asleep.
- Long-term immobility can cause serious complications. Change positions often and take care of your skin. Range-of-motion exercises may help to maintain some muscle tone.
- Splints may help prevent muscle contractures, a condition in which a muscle becomes permanently shortened.
When to Contact a Medical Professional
Muscle paralysis always requires immediate medical attention. If you notice gradual weakening or problems with a muscle, get medical attention as soon as possible.
What to Expect at Your Office Visit
The provider will perform a physical exam and ask questions about your medical history and symptoms, including:
Location:
- What part(s) of your body are affected?
- Does it affect one or both sides of your body?
- Did it develop in a top-to-bottom pattern (descending paralysis), or a bottom-to-top pattern (ascending paralysis)?
- Do you have difficulty getting out of a chair or climbing stairs?
- Do you have difficulty lifting your arm above your head?
- Do you have problems extending or lifting your wrist (wrist drop)?
- Do you have difficulty gripping (grasping)?
Symptoms:
- Do you have pain?
- Do you have numbness, tingling, or loss of sensation?
- Do you have difficulty controlling your bladder or bowels?
- Do you have shortness of breath?
- What other symptoms do you have?
Time pattern:
- Do episodes occur repeatedly (recurrent)?
- How long do they last?
- Is the muscle function loss getting worse (progressive)?
- Is it progressing slowly or quickly?
- Does it become worse over the course of the day?
Aggravating and relieving factors:
- What, if anything, makes the paralysis worse?
- Does it get worse after you take potassium supplements or other medicines?
- Is it better after you rest?
Tests that may be performed include:
- Blood tests (such as CBC, white blood cell differential, blood chemistry levels, and muscle enzyme levels)
- CT scan of the head or spine
- MRI of the head or spine
- Lumbar puncture (spinal tap)
- Muscle or nerve biopsy
- Myelography
- Muscle ultrasound
- Nerve conduction studies and electromyography
Intravenous feeding or feeding tubes may be required in severe cases. Physical therapy, occupational therapy, or speech therapy may be recommended.
References
Kaminski HJ. Disorders of neuromuscular transmission. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 390.
Selcen D. Muscle diseases. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 389.
Warner WC, Sawyer JR. Neuromuscular disorders. In: Azar FM, Beaty JH, eds. Campbell's Operative Orthopaedics. 14th ed. Philadelphia, PA: Elsevier; 2021:chap 35.
Review Date:3/31/2024
Reviewed By:Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997-A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
The Agency for Health Care Administration (Agency) and this website do not claim the information on, or referred to by, this site is error free. This site may include links to websites of other government agencies or private groups. Our Agency and this website do not control such sites and are not responsible for their content. Reference to or links to any other group, product, service, or information does not mean our Agency or this website approves of that group, product, service, or information.
Additionally, while health information provided through this website may be a valuable resource for the public, it is not designed to offer medical advice. Talk with your doctor about medical care questions you may have.

Health Outcome Data
No data available for this condition/procedure.
Read More
Amyotrophic lateral sclerosis (ALS)
Poisoning - fish and shellfish