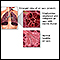
COPD - quick-relief drugs
Description
Quick-relief medicines for chronic obstructive pulmonary disease (COPD) work quickly to help you breathe better. You take them when you are coughing, wheezing, or having trouble breathing, such as during a flare-up. For this reason, they are also called rescue medicines.
The medical name of these medicines is bronchodilators, meaning medicines that open the airways (bronchi). They relax the muscles of your airways and open them up for easier breathing. You and your health care provider can make a plan for the quick-relief medicines that work for you. This plan will include when you should take your medicine and how much you should take.
Follow instructions on how to use your medicines the right way.
Make sure you get your medicine refilled before you run out.
Watch this video about:
Inhaler with spacer - adults
Alternative Names
COPD - quick-relief drugs; Chronic obstructive pulmonary disease - control drugs; Chronic obstructive airways disease - quick-relief drugs; Chronic obstructive lung disease - quick-relief drugs; Chronic bronchitis - quick-relief drugs; Emphysema - quick-relief drugs; Bronchitis - chronic - quick-relief drugs; Chronic respiratory failure - quick-relief drugs; Bronchodilators - COPD - quick-relief drugs; COPD - short-acting beta agonist inhaler
Quick-relief Beta-agonist Inhalers
Quick-relief beta-agonists help you breathe better by relaxing the muscles of your airways. They are short-acting, which means they stay in your system only for a short time.
Some people take them just before exercising. Ask your provider if you should do this.
If you need to use these medicines more than 3 times a week, or if you use more than one canister a month, your COPD probably is not under control. You should contact your provider to see if any changes should be made.
Kinds of Quick-relief Beta-agonists
Quick-relief beta-agonists inhalers include:
- Albuterol (ProAir HFA; Proventil HFA; Ventolin HFA)
- Levalbuterol (Xopenex HFA)
- Albuterol and ipratropium (Combivent Respimat)
Most of the time, these medicines are used as metered dose inhalers (MDI) with a spacer. Sometimes, especially if you have a flare-up, they are used with a nebulizer.
Side effects might include:
- Anxiety.
- Tremor.
- Restlessness.
- Headache.
- Fast or irregular heartbeats. Call your provider right away if you have this side effect.
Some of these medicines also exist in pills, but the side effects are a lot more significant, so they are very rarely used that way.
Quick relief Muscarinic antagonists (anti-cholinergics)
There is one medicine, ipratropium (Atrovent HFA), which works slower than beta-agonists, but faster than other long-acting medicines.
Oral Steroids
Oral steroids (also called corticosteroids) are medicines you take by mouth, as pills, capsules, or liquids. They are not quick-relief medicines, but are often given for 7 to 14 days when your symptoms flare-up. Sometimes you might have to take them for longer.
Oral steroids include:
- Methylprednisolone
- Prednisone
- Prednisolone
References
Anderson B, Brown H, Bruhl E, et al. Institute for Clinical Systems Improvement website. Health Care Guideline: Global Initiative for Chronic Obstructive Lung Disease (GOLD) website. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: 2024 report. goldcopd.org/2024-gold-report/. Accessed May 16, 2024.
Han MK, Lazarus SC. COPD: clinical diagnosis and management. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 6th ed. Philadelphia, PA: Elsevier; 2022:chap 64.
Reilly J. Chronic obstructive pulmonary disease. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 76.
US Department of Veterans Affairs website. VA/DoD Clinical Practice Guideline for The Management Of Chronic Obstructive Pulmonary Disease, Version 3.0, April 2021. www.healthquality.va.gov/guidelines/CD/copd/VADoDCOPDCPGFinal508.pdf. Accessed May 16, 2024.
Waller DG. Asthma and chronic obstructive pulmonary disease. In: Waller DG, ed. Medical Pharmacology and Therapeutics. 6th ed. Philadelphia, PA: Elsevier; 2022:chap 12.
Review Date:5/3/2024
Reviewed By:Allen J. Blaivas, DO, Division of Pulmonary, Critical Care, and Sleep Medicine, VA New Jersey Health Care System, Clinical Assistant Professor, Rutgers New Jersey Medical School, East Orange, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997-A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
The Agency for Health Care Administration (Agency) and this website do not claim the information on, or referred to by, this site is error free. This site may include links to websites of other government agencies or private groups. Our Agency and this website do not control such sites and are not responsible for their content. Reference to or links to any other group, product, service, or information does not mean our Agency or this website approves of that group, product, service, or information.
Additionally, while health information provided through this website may be a valuable resource for the public, it is not designed to offer medical advice. Talk with your doctor about medical care questions you may have.

Care Points
Chronic obstructive pulmonary disease - adults - discharge
COPD - what to ask your doctor
Eating extra calories when sick - adults
How to breathe when you are short of breath
How to use an inhaler - no spacer
How to use an inhaler - with spacer
How to use your peak flow meter